Tim's Story
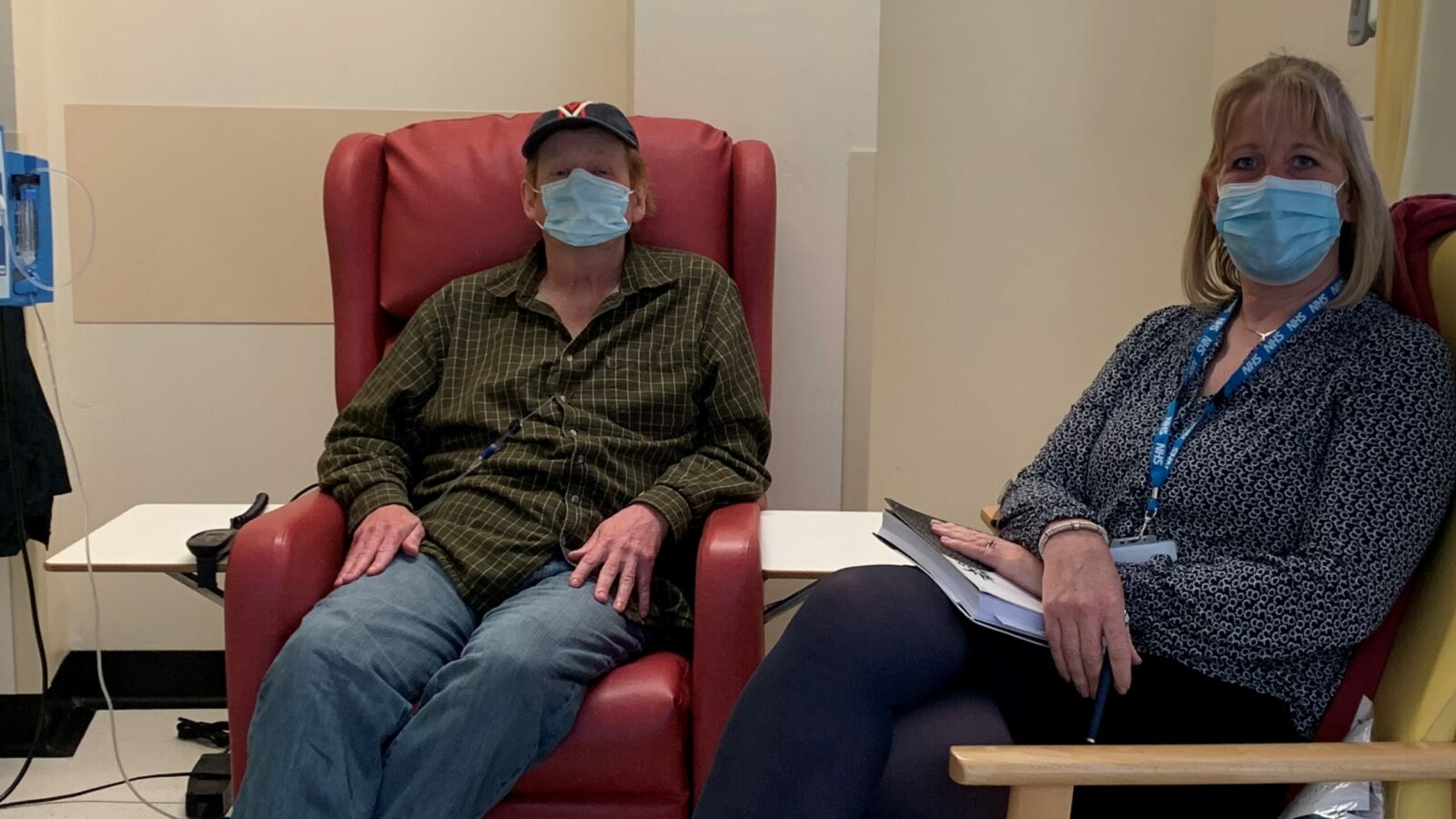
Tim put off going to the doctors for a long time – he talks about his diagnosis and ongoing treatment.
Why not join in one of our brilliant fundraising events? Find out what's coming up next here!
In 2012, I noticed a lump in my left belly; I ignored it generally and continued my life of hard physical work.
Eventually I asked my doctor to take a look at it. Over a two-year period, 2 different doctors looked at it but it wasn’t examined fully. I then noticed a change in my digestion; I began experiencing diarrhoea and constipation, but again I generally ignored these symptoms and put it down to my diet; beer and eating out.
In mid-October 2015, I visited Welshpool practice with bad constipation and pain, and they referred me to Royal Shrewsbury Hospital for colorectal investigations; these were not pleasant, but I’m so glad I went eventually. Later that month, I was diagnosed with colon cancer and terminal lymphatic cancer.
In November, I made a number of visits to the Lingen Davies Centre for discussions and preparations for chemotherapy treatment, with consultants, doctors and nurses including visits to Hamar Centre for videos and conversation.
My chemotherapy treatment began in December; 5 weeks after my diagnosis and was every week thereafter.
In April 2016, I was visiting my relatives in Brighton and developed bad constipation – I was rushed to Royal Sussex hospital and operated on urgently. I had my whole colon removed and a stoma created. I was in hospital for 3 weeks recovering; they had talked about transferring me back to RSH but it proved difficult to arrange. I did eventually return home and I was back at the Lingen Davies Centre 5 weeks after for my last chemotherapy!
Recovery felt like hard work but the loss of the tumor somehow seemed to make me stronger. My lymphoma is a terminal illness, but the chemotherapy has held it in check.
I am very lucky that my experience of nausea and other side effects has been relatively good thanks to the great care given, and my relative youth and fitness. Between 2015 and 2018 I had 7 different PICC lines fitted and got to travel widely with my wife, visiting Greece, Japan and British Columbia Canada. There have been 3 lesser hospital admissions in the last 5 years for infections, and at least 12 scheduled CT Scans.
In March 2018 I had a Portacath fitted in Stoke Hospital that makes for a safer and easier life.
Last year, I took 2 months off from chemotherapy and visiting the Lingen Davies Centre due to the Coronavirus precautions, but I have been attending safely since July 2020 and am nearing my 100th cycle of treatment.
I really feel like I have become part of the family at the Lingen Davies Centre – the nurses are so very kind and friendly…part of their treatment is their optimism that carries us all along.
My wife and I have thrown a number of fundraising events at our home in Welshpool, and many of the chemotherapy nurses have attended and had a great time with us.
Dr Aslan suggested I took counselling support at The Hamar Centre. I would recommend this to anyone with cancer – it allowed me to assess where I had been and how I wished to approach my future. My artistic career and experience is now my focus in life, and I hope to exhibit all my ceramics and art from my lifetime, soon.
I have become inspired, found purpose, and been able make a further contribution to the world, against the odds.

A stoma is an opening on the abdomen that can be connected to either your digestive or urinary system to allow waste (urine or faeces) to be diverted out of your body.
A PICC line is a thin, soft, long catheter (tube) that is inserted into a vein in your arm, leg or neck. The tip of the catheter is positioned in a large vein that carries blood into the heart. The PICC line is used for long-term intravenous (IV) antibiotics, nutrition or medications, and for blood draws.
A portacath is a small chamber or reservoir that sits under your skin at the end of your central line. The other end of the line sits in a large vein close to your heart. You can feel the chamber of the portacath, but unless you’re very thin you can’t usually see it. When you need treatment, your chemotherapy nurse puts a needle into the chamber and gives you injections or attaches a drip. The drugs travel from the chamber to the tubing and into your bloodstream. The portacath stays in place for as long as you need treatment.
Like Tim, many people find it useful to speak to others who are going through the same things as them. There are a range of support groups in our area, some focusing on specific cancers and other more generally.